
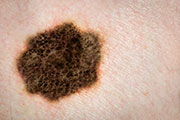
Skin cancer remains the most common cancer for Americans, and invasive biopsies for lesions that could be dangerous melanomas have long been routine.
Now, researchers say they’ve developed a non-invasive test that can spot melanoma skin cancer without a biopsy, according to a new study.
Researchers led by Aneta Stefanovska, of Lancaster University in the United Kingdom, say they’ve used a laser to identify slight differences in blood flow beneath the lesion, which differentiate melanoma from non-cancerous moles.
The test, which takes about 30 minutes, was assessed in 55 people with irregular moles. Follow-up biopsies showed that the test was 100 percent accurate in identifying patients with melanoma.
“We used our knowledge of blood flow dynamics to pick up on markers which were consistently different in the blood vessels supplying malignant moles and those beneath normal skin,” Stefanovska said in a university news release.
The new test “has 100 percent sensitivity and 90.9 percent specificity, which means that melanoma is identified in all cases where it is present, and ruled out in 90.9 percent of cases where it is not,” she added.
Study co-author Marco Rossi of Pisa University in Italy pointed out that “skin malignant melanoma is a particularly aggressive cancer associated with quick blood vessel growth, which means early diagnosis is vital for a good prognosis. The current diagnostic tools of examination by doctors, followed by biopsy, inevitably leads to many unnecessary invasive excisions.”
The new test might “lead to a substantial reduction in the number of biopsies currently undertaken,” Rossi said.
Two melanoma experts in the United States were cautiously optimistic about the test, but said more research is needed.
“The study as presented has many limitations and thus further research is necessary before it could be used in clinical practice,” said Dr. Hooman Khorasani, assistant professor of dermatology at the Icahn School of Medicine at Mount Sinai in New York City.
According to Khorasani, one of the test’s current limitations is the fact that the patient’s blood flow must be monitored for a half-hour. “In a busy dermatology practice in New York City, I believe that collecting data for 30 minutes in a patient exam room would be unrealistic,” he said.
Khorasani also believes that a larger study, with a much wider range of patient types, is needed before confirming the utility of the test.
Dr. Katy Burris is a dermatologist at North Shore-LIJ Health System in Manhasset, N.Y. She said that, “as with many cancers, earlier diagnosis often results in a better outcome, which is what every doctor wants for their patient. But one must remember that this is only one study, and further studies will be needed to determine how accurate this device will be in correctly identifying melanoma.”
The findings were published online earlier this month in the journal Nature Scientific Reports.
More information
The American Cancer Society has more about melanoma.
Source: HealthDay
Copyright © 2024 HealthDay. All rights reserved.

Leave a Reply