
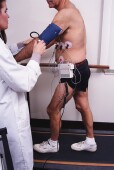
Cardiac rehabilitation programs are considered a key part of recovering from a heart attack — but only a small minority of patients ever attend one, a new study finds.
Of the thousands of older Americans who’d suffered a heart attack in the study, only about 62 percent were referred to a cardiac rehab program, researchers found. And just one-third of those patients actually went.
Cardiac rehab programs include supervised exercise, diet counseling, and help with issues such as quitting smoking and managing medications. Guidelines from the American College of Cardiology say that cardiac rehab should be a standard part of heart attack recovery.
Despite that, research has shown that few patients actually attend the programs. The new study, published in this week’s JAMA Internal Medicine, suggests that the situation is not improving much.
“Participation in cardiac rehab remains disappointingly poor, despite widespread efforts to improve referrals,” said Dr. Jacob Doll, the lead researcher on the study and a fellow at the Duke Clinical Research Institute in Durham, N.C.
The problem is clearly not just related to referrals, Doll said, since two-thirds of patients who were referred to cardiac rehab did not go. And even when they did enroll in a program, he added, few attended the full 36 sessions that are typically covered by insurance.
“Our findings imply that referral isn’t enough,” Doll said. “For many patients, attending cardiac rehab may be too expensive or inconvenient. Others may not understand the importance of cardiac rehab, despite being referred.”
For the study, Doll’s team combed through records from more than 58,000 Medicare patients who were hospitalized for a heart attack between 2007 and 2010. Just over 62 percent were referred to cardiac rehab when they were discharged from the hospital — but only 33 percent of those patients went.
Those who did go were slightly younger and tended to have fewer coexisting health problems, Doll’s team found.
Dr. Patrick O’Gara, a cardiologist at Brigham and Women’s Hospital in Boston, agreed that patients may not understand cardiac rehab’s significance.
In some cases, the doctor or other hospital staff may not fully explain the benefits of cardiac rehab, said O’Gara, who wrote an editorial published with the study.
In other cases, he said, people may find the program overwhelming, since it usually involves three sessions a week for 12 weeks. “For some patients, that commitment is too disruptive or too inconvenient, and it may not be supported by their employer or their family,” O’Gara said.
For elderly patients, he added, transportation can be an obstacle.
Right now, cardiac rehab programs are usually run at hospitals, or sometimes local community centers.
Both Doll and O’Gara said that home-based programs could offer a potential alternative. Studies have been looking at the effects of home programs — which can be done with the help of smartphones — and finding positive results, according to O’Gara.
In the real world, though, home-based rehab is not widely available, Doll said. Even when it is, he added, doctors are not always aware the programs exist, and costs to patients may be higher compared with traditional cardiac rehab.
“We need better ways to provide cardiac rehab services that patients are able to access,” Doll said.
For now, O’Gara said, doctors should be sure they clearly explain the benefits of cardiac rehab, and refer patients to programs as close to home as possible.
He also suggested patients be proactive. “I would encourage patients to have a discussion with their doctor about the benefits of cardiac rehab after hospitalization for a heart-related event,” O’Gara said.
During that talk, he added, patients should bring up any obstacles they could face in sticking with a program.
“As physicians, we need to make it as easy as possible for our patients to attend and complete a cardiac rehab program,” O’Gara said.
More information
The American Heart Association has more on cardiac rehab.
Source: HealthDay
Copyright © 2024 HealthDay. All rights reserved.

Leave a Reply