
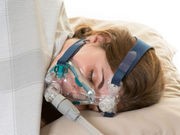
More than half of those diagnosed with sleep apnea fail to stick with the standard treatment for the condition, the CPAP mask, a new study says.
And most aren’t given additional options or referred to a specialist, even when they can’t tolerate the first treatment.
Obstructive sleep apnea is a common breathing disorder in which a person frequently stops or slows their breathing during sleep. The standard treatment is continuous positive airway pressure, or CPAP. A CPAP mask pushes air into the person’s airways while they sleep.
“The most striking thing about our study is that this is the first study to look at how many patients are using CPAP after a diagnosis of obstructive sleep apnea,” said corresponding author Dr. Alan Kominsky, an assistant professor of surgery at Cleveland Clinic in Ohio.
“The surprising finding was just how few patients were referred to other providers once CPAP failed,” he said.
The findings were published recently in the journal Otolaryngology – Head and Neck Surgery.
Obstructive sleep apnea probably affects between 5 percent and 7 percent of the U.S. population, the researchers said. The condition is usually diagnosed during a sleep study that measures how many times someone stops breathing (apnea) or has shallow breathing with a drop in blood oxygen (hypopnea) for at least 10 seconds during each hour of sleep.
The study authors reviewed the medical records of just over 600 people. All of them had been diagnosed with obstructive sleep apnea after a sleep study and were immediately prescribed CPAP.
Just 42 percent began using CPAP regularly as directed. Only about a third of the remaining people who weren’t using CPAP were referred to a specialist to help them manage their sleep apnea.
Dr. Michael Thorpy, director of the Sleep-Wake Disorders Center at Montefiore Medical Center in New York City, said this reflects the difficulty of having patients use CPAP. “It is not an easy treatment for a lot of patients to sleep with a machine at night, and it requires some work and effort to get patients to become compliant,” he said.
Thorpy, who was not involved in the study, found it surprising how few patients in the study were referred to a sleep specialist from the start.
“The thing that strikes me is that they have a pattern of primary care physicians referring the patients to sleep studies, but here [at Montefiore], everybody is seen by a sleep specialist,” Thorpy said. “It’s difficult to get patients to use CPAP, but we work with patients to get the right mask and the right fit and to get the CPAP working for them.”
Sleep centers may have higher rates of people using CPAP because they have sleep specialists working with patients, Thorpy said. “It’s not just a matter of diagnosing a person with sleep apnea and giving them a prescription for a machine and expecting them to use it,” he said.
Respiratory therapists or other care providers can help work with patients or discuss alternatives if a patient is having trouble with CPAP, Kominsky said.
For some, CPAP is the only appropriate treatment, but others may have additional options, including dental devices and surgery, Kominsky said. Dental devices are best for those with mild to moderate sleep apnea, he said.
“Sometimes the problem is reluctance, and a visit with a surgeon to explore the other options will convince the patient to get over their initial refusal to use CPAP,” Kominsky said.
Untreated obstructive sleep apnea increases the risk of heart disease, stroke, high blood pressure and diabetes, as well as memory and thinking trouble, Kominsky said.
More information
For more about sleep disorders, visit the U.S. Centers for Disease Control and Prevention.
Source: HealthDay
Copyright © 2026 HealthDay. All rights reserved.

Leave a Reply